Table of Contents
It is Childhood Epilepsy One of the most common neurological disorders that worries parents is seizures. Seeing a child have a seizure is a frightening experience, but a deep understanding of the condition is the first step toward managing it. In this comprehensive medical guide, we'll delve into the intricacies of this neurological disorder, explaining everything you need to know, from brain physiology to the latest global treatment protocols.
Introduction: Understanding brain electricity and epilepsy
The human brain is a complex network of neurons that communicate via organized electrical signals. When a sudden malfunction or abnormal “electrical storm” occurs in these cells, what we call a brain hemorrhage happens. Seizure.
It is important to distinguish between occasional spasm and illness Epilepsy. Not every child who has a seizure has epilepsy (such as febrile seizures). A child is usually diagnosed with epilepsy if they experience two or more unexplained seizures more than 24 hours apart.
1. Causes of childhood epilepsy: Why does this happen?
There are many underlying causes of epilepsy in children, and in approximately 501 TP3T cases, the cause may remain idiopathic. However, doctors categorize the known causes as follows:
A. Genetic Factors
Genetics plays a pivotal role. A child may inherit a gene that makes them more prone to seizures, or epilepsy may be part of a specific genetic syndrome such as Dravet Syndrome.
B. Structural Injuries (Structural Causes)
Any physical damage to the brain structure can lead to an epileptic focus, including:
- Oxygen deficiency during childbirth.
- Severe head injuries (fall or car accidents).
- Abnormalities in brain development during pregnancy.
C. Metabolic and immunological causes
- Metabolic disorders: A malfunction in the way the body processes sugar or amino acids.
- Infection: Meningitis, viral encephalitis, or parasites.
2. Types of epileptic seizures in children and their symptoms
Epilepsy is primarily classified according to the location in the brain where the seizure begins. This classification is essential for determining the appropriate treatment.
First: Focal Seizures
It begins in one specific area of the brain.
- Focal seizures with consciousness: The child remains awake and may experience strange sensations, imaginary smells, or involuntary movements in one hand or leg.
- Focal seizures with impaired consciousness: The child may appear “daydreaming” or staring into space, and may make repetitive movements (such as rubbing hands or chewing).
Second: Generalized Seizures
It involves electrical activity in both hemispheres of the brain from the very beginning.
- Absence Seizures: It was called "minor epilepsy." The child would suddenly stop moving and stare blankly for a few seconds. It was often mistakenly thought to be a lack of attention at school.
- Tonic-clonic seizures: Formerly known as "grand mal seizures," the child loses consciousness, their body stiffens (tonatory phase), and then they begin to convulse (clonic phase). This is the typical picture of epilepsy.
- Atonic attacks: A sudden loss of muscle tone, leading to the child suddenly falling (Drop attacks).

3. Epilepsy diagnosis: How does the doctor confirm it?
Accurate diagnosis is the cornerstone of successful treatment. Pediatric neurologists rely on the following tools:
Detailed medical history
Describing the seizure is the most important tool. (Family video recording of the seizure helps the doctor tremendously).
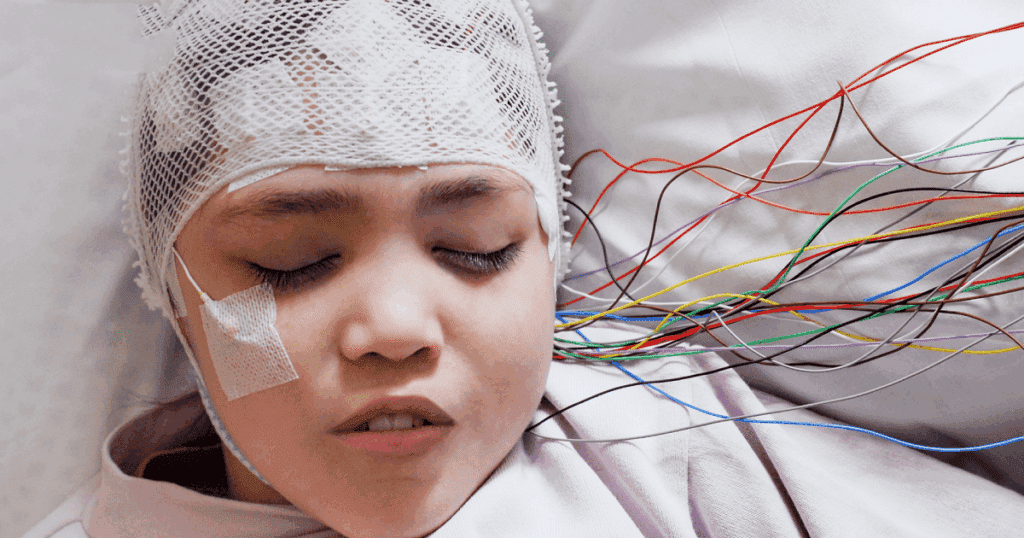
Electroencephalography (EEG)
This is the most important test. Electrodes are placed on the scalp to record electrical waves.
- It can be performed while the child is awake or asleep.
- It reveals “electrical spikes” or epileptic foci.
Magnetic resonance imaging (MRI)
It is used to detect any structural abnormalities, tumors, or scars in the brain that may be the cause of the seizures.
Blood and genetic tests
To rule out metabolic causes or to identify rare genetic syndromes.
4. Modern treatment options for childhood epilepsy
The goal of the treatment is “zero seizures” (Seizure Freedom) with minimal side effects.
A. Drug therapy (Antiepileptic Drugs – AEDs)
It is the first line of treatment. The medication is successful in controlling seizures in approximately 701 TP3T children.
- Common examples: Levetiracetam (Keppra), sodium valproate (Depakine), carbamazepine (Tegretol).
- Important advice: Adhering to the prescribed dosages is the secret to success.
B. The Ketogenic Diet (Keto Diet)
When medications fail, doctors may resort to the ketogenic diet. This is a very high-fat, very low-carbohydrate diet that forces the brain to use ketones as fuel instead of glucose, effectively reducing seizures in cases of intractable epilepsy.
c. Vagus nerve (VNS) stimulation
A small device, similar to a pacemaker, is implanted under the skin in the chest, sending electrical pulses to the vagus nerve in the neck to calm brain activity.
Dr. Epilepsy Surgery
The last option for complex cases that do not respond to medication and where the seizures are caused by a specific and safe area for removal in the brain.
5. First aid for an epileptic seizure: What to do?
This information could save a life, so every parent and teacher should know it.
✅ Do:
- Stay calm and time your shift.
- Keep any sharp or hard objects away from the child.
- Place something soft under his head.
- Turn the baby onto their side (recovery position) as soon as the convulsion stops to facilitate breathing.
❌ Do not:
- no Putting anything in a child's mouth (he won't swallow his tongue, that's a medical myth).
- no She tries to forcibly restrain the child to prevent movement.
- no Give him water or medicine during the seizure.
When should you call an ambulance?
- If the attack lasts more than 5 minutes.
- If the seizures recur without regaining consciousness in between.
- If the seizure occurs in the water.
- If the child sustains a serious injury during the fall.

6. Living with epilepsy: school, sports, and mental health
A child with epilepsy is a normal child who should not be deprived of his childhood.
- At school: The school administration and nurse should be informed about the child's condition, the type of seizures, and how to manage them. In most cases, epilepsy should not affect intelligence.
- Sports: Children are encouraged to participate in sports (with some caution in swimming and climbing heights where supervision is necessary).
- Psychological support: Anxiety and depression can accompany epilepsy, whether due to medication or social stigma. Family support is a child's strongest defense.
conclusion
If your child is diagnosed with Childhood epilepsy This is not the end, but rather the beginning of a treatment journey that requires patience and awareness. With the tremendous advancements in medicine, the vast majority of children live completely normal lives, and a significant percentage even outgrow seizures and medication as they get older (what is called "epilepsy remission"). Always consult your doctor, and don't hesitate to ask for support.
Frequently Asked Questions (FAQ) – To boost your visibility in Google Snippets
1. Can a child be completely cured of epilepsy? Yes, statistics indicate that a large number of children grow out of epilepsy, especially if the seizures are controlled with medication and there is no permanent structural cause in the brain.
2. Does epilepsy affect a child's intelligence? In most cases of idiopathic epilepsy, a child's intelligence is perfectly normal. However, very frequent and uncontrolled seizures, or the side effects of some strong medications, may temporarily affect concentration.
3. Is it possible For the child Can someone with epilepsy use tablets and mobile phones? Yes, but in moderation. There is a rare type called photosensitive epilepsy that is affected by flashing lights, but it doesn't affect all people with epilepsy. It's advisable to reduce screen time and ensure the room is well-lit.

