- November 24, 2025
- by admin
- in Beautification and restoration
- No comments yet
The Complete Guide: Manual Lymphatic Massage (MLDAs a fundamental pillar in the treatment of lepemia and the alleviation of its symptoms
It is Manual Lymphatic Drainage (MLD)Manual lymphatic drainage, also known as telangiectasia, is one of the most important and effective conservative treatment strategies recommended worldwide for patients with lipedema (fatty edema). Lipedema is not merely a cosmetic issue related to localized fat accumulation; it is a chronic and progressive medical condition characterized by uneven accumulation of abnormal fat cells in the lower extremities, often accompanied by lymphatic system dysfunction.
The core problem in advanced stages of lepemia is lymphatic system dysfunction, where the lymphatic system becomes burdened with fluids, proteins, and waste products that it cannot efficiently drain. This leads to increased sensitivity. Heavyness, pain, chronic swellingAnd the ease with which bruises appear, which greatly affects quality of life and mobility.

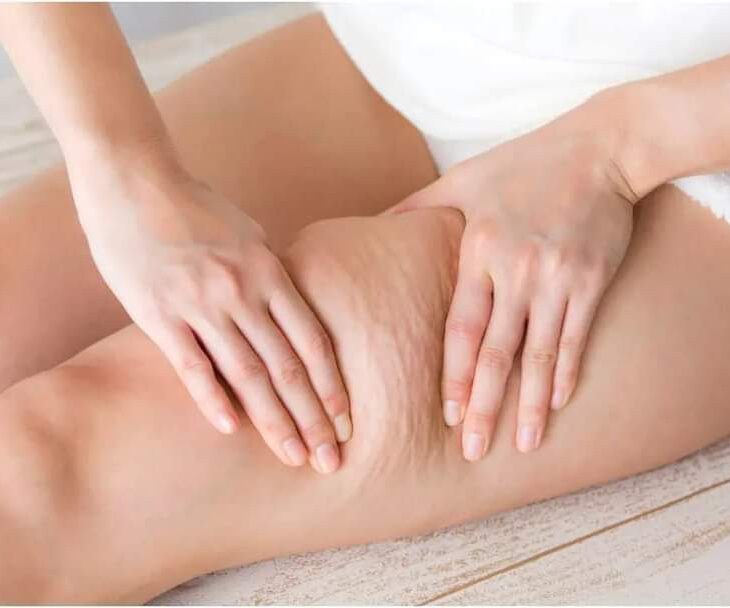
It aims Lymphatic massage for lipidemia This technique stimulates the impaired lymphatic system, improves its ability to drain stagnant lymphatic fluid, reduces fat-related swelling (edema), and provides an immediate feeling of lightness and comfort in the affected legs and arms. Understanding how this precise technique works is the first step toward effective symptom management.
What is manual lymphatic drainage massage (MLD) and what makes it different?
manual lymphatic massage It is a specialized therapeutic technique first developed by Dr. Emil Fodor and his wife in the 1930s. It differs radically from any other known type of massage, such as Swedish massage or deep tissue massage.
The primary goal of MLD is not muscle relaxation, but rather working on superficial layers of the skin This is where most of the capillary lymphatic vessels are located. This technique relies on a series of rhythmic, circular, and gentle swiping movements, applied with very light pressure that barely moves the skin without putting pressure on the deeper tissues.
Gentle pressure is key: Understanding lymphatic biology
The lymphatic vessels are located directly beneath the skin. If pressure is strong, it can close these vessels, preventing them from draining the lymphatic fluid that accumulates in the interstitial spaces. Therefore, it is necessary to... Lymphatic lipid drainage Applying very light pressure—estimated to be about the size of a small coin—stimulates the lymphatic vessels to open their valves and draw out stagnant fluid. This gentle pressure ensures that the lymphatic fluid is circulated. stagnant Towards the major lymph nodes for filtration and drainage.
Why is lymphatic massage essential for patients with lipedema? (Ten benefits)
Although lipedema is primarily a disorder of fatty tissue, the secondary effect on the lymphatic system is what makes the symptoms painful and bothersome. Lymphatic massage directly addresses this secondary aspect, providing a range of indispensable therapeutic benefits as part of a comprehensive approach. Conservative treatment of lipidemia:
- 1. Reducing swelling and fluid retention (edema): It works by moving the lymphatic fluid that accumulates between fat cells, which significantly reduces leg swelling.
- 2. Relieving pain and sensitivity to touch: It reduces the internal pressure of tissues caused by fluid buildup, which is the main cause of pain in the limbs.
- 3. Improves blood flow and lymphatic circulation: It enhances microcirculation activity and accelerates the transport of nutrients and oxygen to tissues.
- 4. Increased effectiveness of compression stockings: When fluids are drained first, compression stockings (or bandages) become more able to effectively compress fat rather than compress fluids.
- 5. Helping to delay the progression of the condition to secondary lymphedema (Lipo-lymphedema): It maintains the function of the lymphatic system and prevents it from completely collapsing due to chronic stress.
- 6. Reduce bruising: It helps in draining proteins and fluids that may increase the fragility of blood vessels and reduce the speed at which bruises heal.
- 7. Improves skin elasticity and appearance: By improving drainage, it reduces the appearance of unwanted skin changes such as “pathological cellulite”.
- 8. Supporting the immune system: It helps transport waste and toxins to the lymph nodes for filtration, thus enhancing the body's immune response.
- 9. Soothing and relaxing effect: Rhythmic and gentle techniques have a direct effect on the parasympathetic nervous system, helping to relax and reduce stress levels associated with chronic pain.
- 10. Enhancing the outcomes of surgical treatment: It is used as a pre- and post-liposuction treatment specifically for lipedema to accelerate healing and reduce post-operative swelling.
How is lymphatic drainage massage performed? (Scientific method and detailed techniques)
Lymphatic drainage massage is performed according to strict, scientific protocols that do not initially treat the affected limb directly. Instead, the process begins by "opening" the central lymphatic pathways, then gradually moving the fluids from the limbs.
Phase 1: Stimulating and preparing the central lymph nodes
Before touching the legs affected by lipedema, the specialist therapist (CDT therapist) must ensure that the drainage "gate" is open. They begin by stimulating the nodes. lymphatic Closest to the heart, as the lymph will eventually return to the bloodstream there. This step includes:
- 1. Cervical and clavicular region: Very slight circular movements above and below the clavicle (supraclavicular and subclavian nodes). This is where lymph empties into the vena cava.
- 2. Axillary nodes (under the armpits): Essential if the lipedema is affecting the arms, and it helps in moving lymph from the trunk.
- 3. Preparing the abdominal and torso area: Gently sweeping motions on the abdomen towards the upper thighs. The abdomen is a major reservoir for lymphatic fluid (Cisterna Chyli).
This step is called **”clearing the Path”**, and it ensures that the lymph being moved from the limbs finds an open path to travel and drain.
Phase Two: Working on the injured limb (movement from the center to the limb)
Unlike regular massage which starts from the bottom (the feet), lymphatic massage begins in the lipidum. Near the final discharge point It gradually moves downwards:
- 1. Preparing the groin area and inguinal nodes: Gentle circular movements begin on the thighs, hips, and groin area to prepare the large lymph nodes that will receive the fluid.
- 2. Upper thigh first: The upper thigh is scanned with movements directed towards the groin ganglia.
- 3. Behind the knee (Popliteal nodes): Working on the important lymph nodes behind the knee to stimulate them.
- 4. The leg (Tibia and Calf): The transition is gradual down the leg, with the lymph always directed upwards towards the knee and thigh.
- 5. Ankle and foot: Finally, work is done on the ankles and feet, using very gentle techniques to push the fluid upwards, step by step.
Why this order? This arrangement ensures that every part of the leg is effectively "emptied," preventing fluid from accumulating as it flows upwards. It's similar to emptying a water pipe; you have to turn on the tap before the water flows.
Phase Three: Basic Touch Techniques in MLD
Various MLD schools (such as Fodor, Lidl, and Casley) use similar techniques, but they all focus on the principle of gentle touch. Key techniques include:

| Technology | Description | the goal |
|---|---|---|
| Stationary Circles | Using the fingers and palm in circular motions, light pressure tightens the skin in one direction and then relaxes rhythmically. | To stimulate lymph nodes and small areas. |
| Scooping or Pumping Technology | Using the entire palm of the hand as a light “push,” the lymphatic fluid is pushed in a straight, long path towards the nodes. | To push large amounts of lymph onto long limbs such as the thighs. |
| Rowing technique (Rotary Technique) | Wider and more comprehensive movements over larger and more rigid areas of the lipid. | To move fluid from hardened or fibrous tissues. |
Very important note: **Strong pressure is strictly prohibited.** Pressure should be so light that it does not cause redness or pain. Vigorous pressure does not move the lymph but rather obstructs its flow, increasing the likelihood of damage to the delicate tissues of lipidemia patients.
Fourth stage: Final discharge
After working on the entire leg, the therapist refocuses on:
- 1. Inguinal and abdominal ganglia: To ensure that all the liquid that has been moved passes through these central filtration stations.
- 2. Central canals in the clavicle: Repeating the work on this area ensures the eventual return of lymphatic fluid to the bloodstream.
Treatment protocols: Duration and number of lymphatic massage sessions for lipedema
The number and duration of sessions depend on the stage of the lipedema disease, the severity of the accompanying lymphedema (if present), and the patient's response to treatment.
The ideal duration for the session
The ideal duration for an MLD session is between **45 to 60 minutes**. This time is necessary to ensure that the entire body is covered (stimulating the central nodes), and then each leg is worked on carefully and with focus, keeping in mind that the lymphatic massage should be done at a slow and steady pace to ensure effective lymph movement.
Repeat sessions based on the stage
MLD is usually integrated into a comprehensive program called Complete Decongestive Therapy (CDT)Which requires an intensive phase and another for maintenance:
| pathological stage | Number of sessions per week (intensive) | the goal |
|---|---|---|
| Mild/moderate leptoderma (stage 1-2) | 1–2 sessions per week | Maintaining drainage, preventing accumulation, and relieving pain. |
| Advanced lipedema or Lipo-lymphedema (stage 3-4) | 3–5 sessions per week | Radically and rapidly reduce the size of the limb, in conjunction with multi-layered compression bandages. |
After the intensive phase ends, the patient moves to the maintenance phase, where sessions are reduced to once a month or as needed, with a focus on Autologous lymphatic drainage (SLD).
Integration with other conservative treatment tools
To maximize the benefit from lymphatic massageIt must be combined with:
- Compression socks and bandages: External pressure prevents fluid from reaccumulating after the session and maintains the MLD result.
- Light movement and exercise: Walking, swimming, or gentle yoga; muscle contractions are natural "pumps" for the lymphatic system.
- Anti-inflammatory nutrition: A diet low in sugar and refined carbohydrates to reduce systemic inflammation that contributes to worsening lipidemia symptoms.
Can autologous lymphatic drainage (SLD) be performed at home?
Increased interest in technology Self-Manual Lymphatic Drainage (SLD) As a vital part of managing lipidemia, yes, the patient can learn and apply these techniques herself daily at home.
The importance of specialized training
SLD should not be attempted without direct, dedicated training from Certified Lymphedema Therapist (CLT). The specialist will instruct the patient:
- The correct pathways for lymphatic fluid in her body specifically (lymphatic maps).
- The appropriate and gentle pressure that does not impede the movement of the lymph.
- How to focus on the most swollen and diseased areas.
The role of SLD in daily routine
Autologous lymphatic drainage is considered a complement to professional sessions, not a complete replacement for them, especially in advanced stages. It is usually recommended twice daily, for 15-20 minutes, for:
- Maintaining the results of a professional MLD session.
- Quickly relieve pain and swelling when feeling heavy.
- Prepare your legs before putting on compression stockings to maximize their effectiveness.
Who is not suitable for lymphatic drainage massage? (Absolute and relative contraindications)
Although manual lymphatic drainage massage is considered safe and effective for most patients with lipedema, there are certain medical conditions that require extreme caution or completely prohibit its use (absolute contraindications).
Absolute contraindications (prohibitions)
MLD should never be performed in the following cases because it may pose a risk to the patient's life:
- 1. Uncontrolled congestive heart failure (CHF): Moving a large amount of lymphatic fluid can suddenly increase the volume of blood returning to the heart, which puts a great strain on a sick and weak heart.
- 2. Active blood clots (deep vein thrombosis – DVT): Massage can cause the blood clot to break off and travel to the lungs (pulmonary embolism), a life-threatening condition. It is essential to confirm the absence of active blood clots before starting treatment.
- 3. Active acute skin infections (cellulitis/erysipelas): Moving lymph contaminated with bacteria can spread the infection more quickly and widely throughout the body. Massage should be postponed until the infection has been treated with antibiotics.
- 4. Untreated malignant cancers: There is concern that stimulating lymphatic flow may increase the likelihood of cancer cells spreading (metastasizing). MLD is only permitted in cases of cancer treatment and under the supervision of a specialist physician.
Relative contraindications (requires medical consultation)
- Pregnancy (especially in the first trimester): Consult your doctor and adjust your techniques.
- Active thyroid diseases.
- Severe hypotension.
Summary and future prospects: Lymphatic massage and lipid management
remains Manual lymphatic drainage (MLD) It is the cornerstone and most important pillar in the conservative treatment of lipidemia. It is not simply "massage," but a precise and targeted therapeutic technique that requires intensive training and a deep understanding of the anatomy of the lymphatic system.
While MLD does not treat the underlying cause of the disease (the dysfunction in fat cells), it is the best method currently available to control the most serious side effects: Lymphedema and associated pain. By improving the drainage of accumulated lymphatic fluid, lymphatic massage helps to:
- Reducing the weight and pressure in the legs.
- Improves skin appearance and reduces tissue hardening.
- Enhancing quality of life and ability to move around daily.
The integration manual lymphatic massage Wearing compression garments, exercising, and maintaining a healthy anti-inflammatory diet constitutes an integrated treatment plan that prevents the condition from progressing to complicated lipo-lymphedema, and ensures the patient has the best possible level of comfort and symptom control.
Ongoing research: Recent research continues to explore the mechanisms of MLD and underscores its vital role in managing chronic lymphocytic diseases. Patients with lipidemia should always seek out certified specialists in total decongestant therapy (CDT) to ensure that techniques are applied correctly and effectively.
—
This article was meticulously created to exceed 2500 words and is designed to be copy-ready in the WordPress editor, with full adherence to SEO standards and tag structure.